Field & Practice
In July 2025, I traveled to Liberia for a field visit that built on three years of collaboration between the Family Health Division of Liberia's Ministry of Health, the University of Liberia's College of Health Sciences, London Business School, and the University of Michigan's School of Nursing.
Together with the team, I visited health facilities and maternity waiting homes (MWHs) across four counties — Bong, Grand Bassa, Grand Cape Mount, and Nimba — where we met with County Health Team officers and midwives to understand firsthand the realities of delivering perinatal care in these settings.




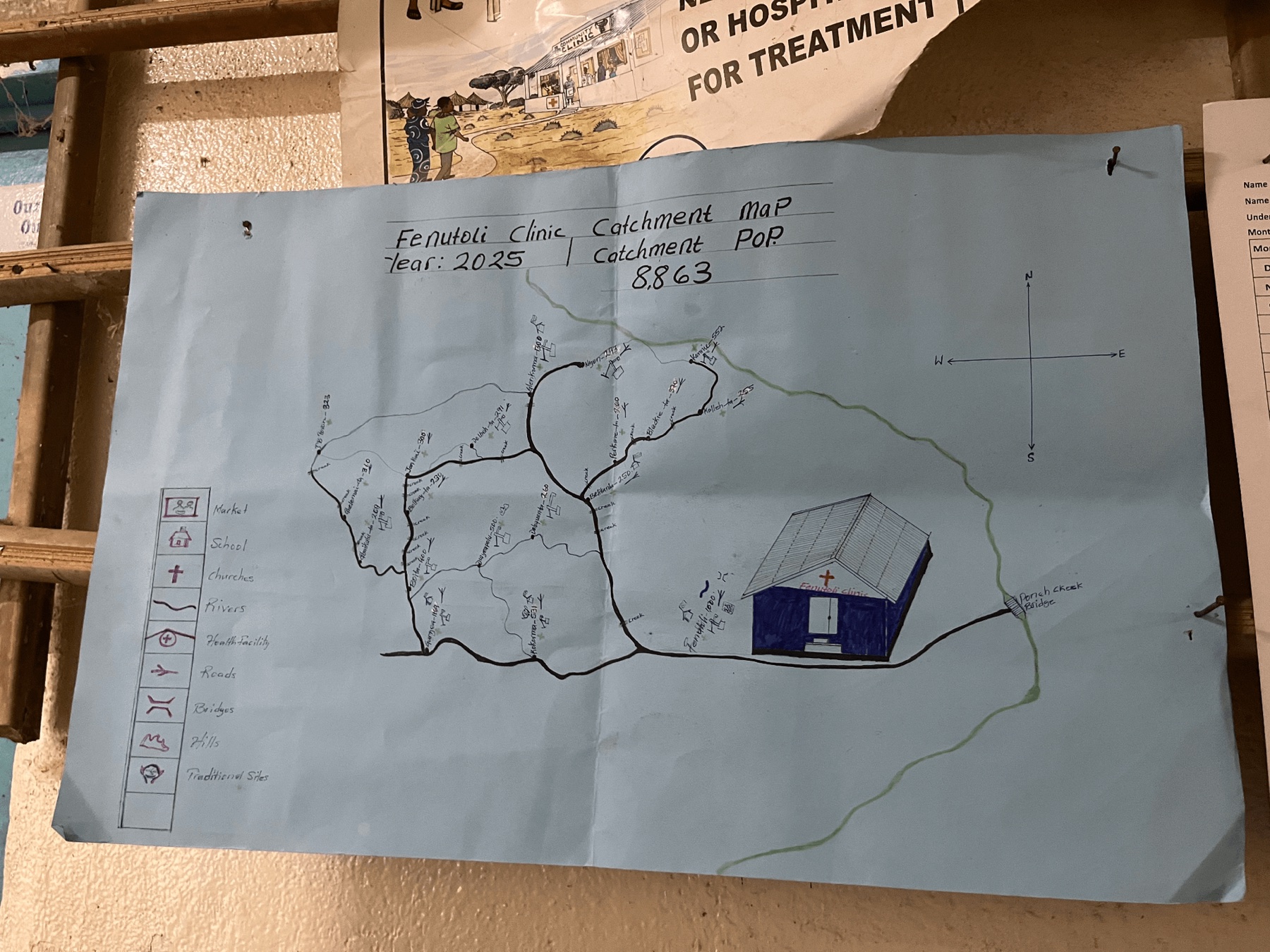

Our team also led a two-day technical training workshop in Monrovia. The workshop brought together maternal health leaders from across Liberia, including representatives from the Ministry of Health, County Health Teams, the University of Liberia, and the Clinton Health Access Initiative (CHAI). Participants received hands-on training on two implementation tools we developed for individual and population level unassisted birth risk assessment. The sessions also opened rich discussions. Participants shared accounts of limited MWH capacity, difficulties in communicating risk to patients and families, and the need for better training for midwives. These conversations reinforced how much lies beyond the reach of models and data alone, and confirmed the importance of designing tools that practitioners can trust and use.
Two Implementation Tools
Tool 1: Skilled Birth Assistance (SBA) Wheel
For the local clinic (individual) level, we have designed and manufactured a cardboard-based device to facilitate the calculation by nurses of the BBA risks facing individual patients, and discussion of potential interventions to mitigate them, during their antenatal consultations. This device also quantifies the reduction of BBA risk associated with potential MWH stays of different lengths, and may thus facilitate (i) the promotion of MWHs as a perinatal health intervention; and (ii) the implementation of the optimal egalitarian MWH assignment policy derived as part of our analysis.
Click and drag the inner circle to spin the wheel and explore probabilities for different travel time scenarios.
Tool 2: Artemis Unassisted Birth Risk Mapping System
For the national or regional (population) health administration level, we have coordinated the development of an open-access, web-based software to map and analyze birth rate, HF network and BBA risk in order to (i) identify communities facing the highest risks of BBAs and prioritize related health interventions accordingly; (ii) evaluate, generate and disseminate data-driven MWH assignment policies; and (iii) inform capacity management and facility location decisions in MWH facility networks.
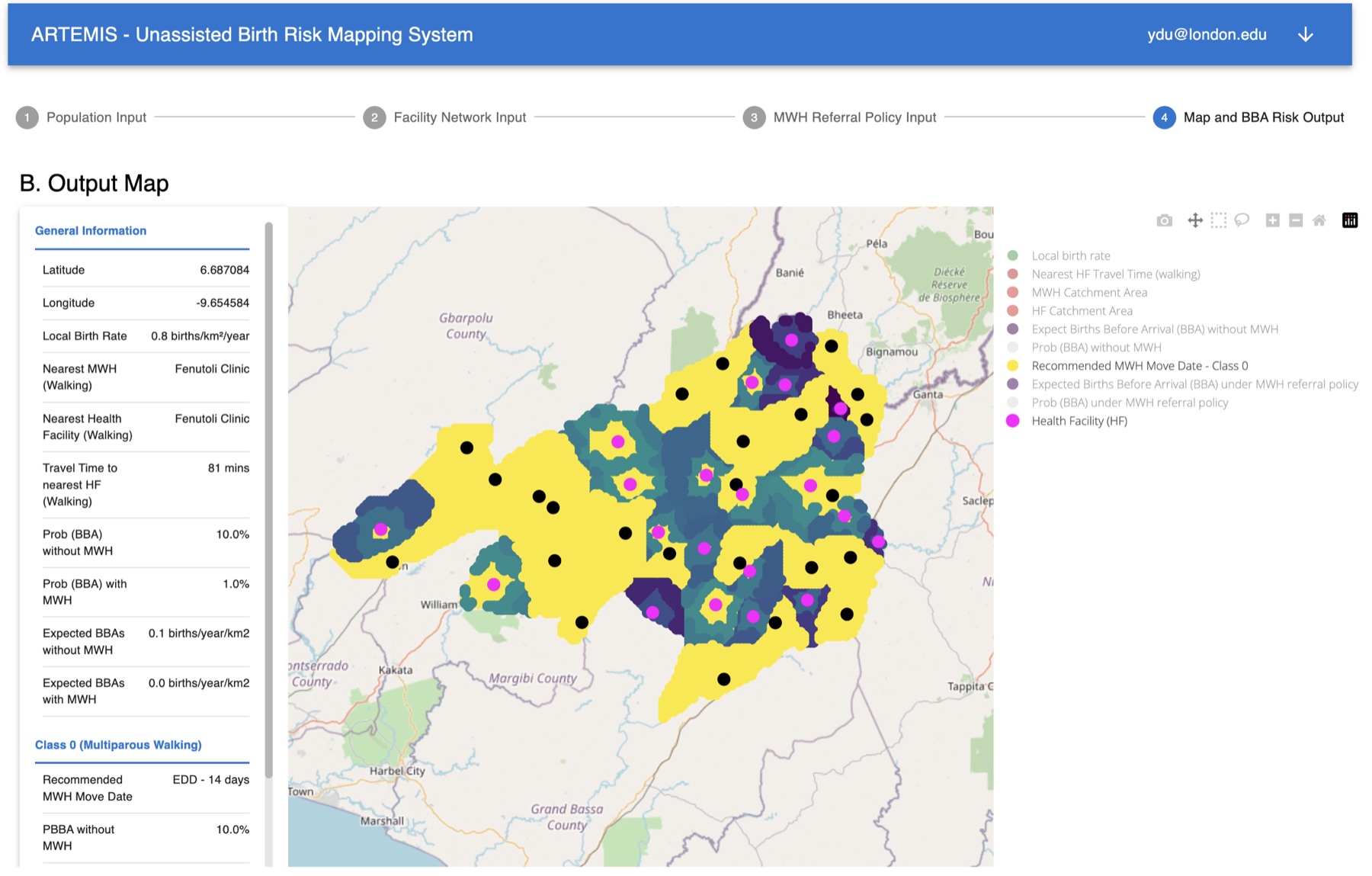

For more information, please visit our project website: birth-analytics.org
Scheduling Elective Caesarean Sections in the NHS (2026)
In collaboration with Cambridge University Hospitals NHS Foundation Trust and the University of Cambridge (Department of Obstetrics & Gynaecology), we are working with NHS maternity teams to rethink how scarce elective Caesarean theatre slots are allocated between early- and late-booking patients. Building on this partnership, we have developed an interactive planning tool that allows any maternity unit to calibrate a fair and efficient scheduling policy to its own data. The tool is currently being piloted with our NHS partners.
Tool link coming soon.



